Summarize this blog post with: ChatGPT | Perplexity | Claude | Grok
Kidney failure treatment decisions can feel overwhelming, especially when doctors mention dialysis and kidney transplant as the main options. You’ve probably already heard that both treatments can keep patients alive, but the real differences in survival, lifestyle, recovery, and long-term costs are often unclear. In this guide, we’ll explain dialysis vs kidney transplant in simple terms so you can make a more informed and confident healthcare decision.
Key Takeaways
- Dialysis is a life-sustaining treatment that removes waste and excess fluid when kidneys stop functioning properly.
- Kidney transplantation replaces a failed kidney with a healthy donor kidney and may improve long-term survival and quality of life.
- Hemodialysis usually requires treatment sessions three times weekly, while transplant recipients need lifelong anti-rejection medications.
- Kidney transplants generally offer better long-term survival rates and fewer lifestyle restrictions for eligible patients.
- Dialysis may still be the safest option for patients who are not medically eligible for transplant surgery.
- Long-term dialysis costs can exceed transplant costs despite dialysis having lower upfront expenses.
- Early consultation with a nephrologist improves treatment outcomes and helps patients prepare for future transplant opportunities.
What Is the Difference Between Dialysis and Kidney Transplant?
Dialysis and kidney transplant are two different treatments for end-stage kidney disease (ESRD). Dialysis artificially filters waste and excess fluid from the blood, while a kidney transplant surgically replaces a failed kidney with a healthy donor kidney.
First, dialysis works as an external support system for kidneys that no longer function properly. For example, hemodialysis machines clean the blood several times per week to remove toxins and maintain electrolyte balance. This treatment can help patients survive for years, but it does not restore natural kidney function.
At the same time, a kidney transplant restores kidney function by placing a healthy donor kidney inside the patient’s body. For example, a kidney from a living donor may function for 15–20 years on average. — Source: National Kidney Foundation, 2024
Dialysis is a medical treatment that removes waste products and excess fluid from the blood when the kidneys can no longer function properly.
A kidney transplant is a surgical procedure that replaces a failed kidney with a healthy kidney from a living or deceased donor.
How Does Kidney Failure Lead to Dialysis or Transplant?
Kidney failure occurs when the kidneys lose most of their filtering ability. This condition is commonly caused by diabetes, high blood pressure, chronic kidney disease, or inherited disorders.
Moreover, untreated kidney failure can cause dangerous toxin buildup, swelling, anemia, heart complications, and fluid overload. For example, many ESRD patients develop fatigue, nausea, breathing difficulties, and reduced urine output before requiring dialysis or transplant.
According to the National Kidney Foundation, millions of people worldwide live with chronic kidney disease, and many eventually progress to kidney failure. — Source: National Kidney Foundation, 2024
Why Does Choosing the Right Kidney Failure Treatment Matter?
Choosing the right kidney failure treatment affects survival, quality of life, financial burden, and long-term health outcomes.
First, dialysis and transplant differ significantly in how they affect daily life. For example, dialysis patients often follow strict treatment schedules and dietary restrictions, while transplant recipients usually regain more freedom after recovery.
Second, treatment selection influences long-term survival rates. A large comparative study found that kidney transplant recipients generally experience lower mortality rates than long-term dialysis patients after the early post-surgery period. — Source: Clinical Kidney Journal, 2017
Additionally, emotional and financial stress also vary between treatments. For example, long-term dialysis may require multiple hospital visits weekly, while transplant patients face surgery risks and lifelong medication costs.
Kidney transplantation generally provides better long-term survival and quality of life than long-term dialysis for eligible patients.
How Does Dialysis Work for Kidney Failure Patients?
Dialysis works by filtering waste products, toxins, and excess fluids from the blood when the kidneys stop functioning effectively.
First, dialysis is divided into two major types:
- Hemodialysis
- Peritoneal dialysis
Each method supports kidney function differently.
What Is Hemodialysis?
Hemodialysis is a treatment that uses a machine and artificial filter to clean the blood outside the body.
Typically, patients visit a dialysis center three times weekly. Each session often lasts around four hours.
Hemodialysis typically requires treatment sessions three times per week, with each session lasting around four hours.
For example, many patients schedule dialysis on alternating days to manage toxin levels consistently.
At the same time, hemodialysis may cause:
- Fatigue
- Low blood pressure
- Muscle cramps
- Headaches
- Infection risks at access sites
What Is Peritoneal Dialysis?
Peritoneal dialysis is a home-based dialysis method that uses the abdominal lining to filter waste from the blood.
Unlike hemodialysis, this method allows patients greater flexibility because it can be performed at home.
For example, some patients use automated machines overnight while sleeping. This approach may improve convenience for working adults or elderly patients with transportation challenges.
Advantages of Dialysis
Dialysis offers immediate life-saving treatment for kidney failure patients.
Key benefits include:
- Widely available treatment centers
- No major surgery required initially
- Suitable for patients ineligible for transplant
- Useful while waiting for donor kidneys
Additionally, dialysis often becomes the first treatment before transplant eligibility evaluation.
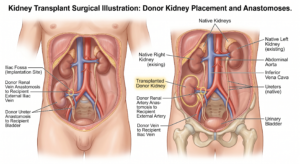
What Happens During a Kidney Transplant Procedure?
A kidney transplant procedure involves surgically placing a healthy donor kidney into a patient with kidney failure.
First, donor kidneys may come from:
- Living donors
- Deceased donors
Living donor kidneys often last longer and function more quickly after surgery. According to the National Kidney Foundation, living donor kidneys may function for 15–20 years on average. — Source: National Kidney Foundation, 2024
Who Is Eligible for a Kidney Transplant?
Kidney transplant eligibility depends on overall health, age, medical history, and the ability to tolerate surgery.
For example, patients with severe heart disease, uncontrolled infections, or active cancer may not qualify immediately.
Moreover, doctors usually evaluate:
- Heart health
- Diabetes control
- Infection risks
- Weight management
- Psychological readiness
What Is Recovery Like After Kidney Transplant?
Kidney transplant recovery usually takes several weeks to several months depending on patient health and complications.
First, transplant recipients require close monitoring to detect rejection signs early. Additionally, lifelong immunosuppressant medications are necessary.
Kidney transplant recipients usually require lifelong immunosuppressant medications to prevent organ rejection.
For example, common medications include tacrolimus and corticosteroids to suppress immune system attacks on the donor kidney.
Is Kidney Transplant Better Than Dialysis for Long-Term Survival?
Kidney transplantation generally provides better long-term survival outcomes than long-term dialysis for eligible patients.
According to research published in Clinical Kidney Journal, transplant recipients had significantly lower death rates compared with dialysis patients after the initial recovery period. — Source: Clinical Kidney Journal, 2017
Additionally, studies show that transplant recipients often experience improved cardiovascular health and lower infection-related mortality compared with dialysis patients.
Survival Comparison Table
|
Factor |
Dialysis |
Kidney Transplant |
|---|---|---|
|
Long-term survival |
Lower overall |
Higher overall |
|
Early treatment risk |
Lower surgical risk |
Higher short-term surgical risk |
|
Lifestyle freedom |
Limited |
Greater flexibility |
|
Need for hospital visits |
Frequent |
Less frequent after recovery |
|
Daily dietary restrictions |
Strict |
Moderate |
|
Long-term health outlook |
Progressive complications possible |
Better quality-adjusted survival |
Furthermore, research from MUSC Health reports that patients living with transplanted kidneys for 10 years demonstrate greater survival rates than long-term dialysis patients. source
Kidney transplant patients typically live longer than patients who remain on dialysis long-term.
Are There Situations Where Dialysis Is Better?
Dialysis may be safer than transplant surgery for patients with severe medical complications or advanced frailty.
For example, elderly patients with multiple cardiovascular conditions may face increased surgical risks during transplantation.
That being said, dialysis often serves as a temporary bridge while patients wait for donor kidneys.
How Does Quality of Life Compare Between Dialysis and Kidney Transplant?
Quality of life is generally higher after successful kidney transplantation compared with long-term dialysis.
First, transplant recipients usually regain greater independence. For example, many patients return to work, travel more easily, and experience fewer food restrictions after recovery.
At the same time, dialysis schedules can significantly affect daily routines. Patients often spend 12–15 hours weekly receiving treatment.
According to observational studies, transplant recipients report better physical and emotional health scores compared with dialysis patients. — Source: PMC Observational Study, 2022
Lifestyle Restrictions on Dialysis
Long-term dialysis often requires strict dietary and fluid management.
Common restrictions include:
- Reduced potassium intake
- Fluid limitations
- Controlled phosphorus consumption
- Frequent medical appointments
Long-term dialysis may involve strict fluid restrictions, dietary limitations, and higher rates of cardiovascular complications compared to transplantation.
Daily Life After Kidney Transplant
Life after kidney transplant is often more flexible but still requires medical monitoring and medication adherence.
For example, transplant recipients must:
- Take medications consistently
- Attend regular follow-up visits
- Avoid infections carefully
However, many patients report improved energy levels and better social functioning after successful transplantation.
How Much Does Dialysis Cost Compared to Kidney Transplant in India?
Dialysis usually has lower upfront costs, while kidney transplant often becomes more cost-effective over the long term.
In India, dialysis costs can accumulate significantly because treatment continues indefinitely.
Estimated Cost Comparison in India
|
Treatment |
Approximate Cost |
|---|---|
|
Hemodialysis per session |
₹2,000–₹5,000 |
|
Monthly dialysis cost |
₹25,000–₹60,000 |
|
Kidney transplant surgery |
₹5 lakh–₹12 lakh |
|
Post-transplant medicines |
₹10,000–₹25,000 monthly |
Additionally, some Indian government programs now provide subsidized or free dialysis sessions in public hospitals.
A recent healthcare analysis found that kidney transplantation often becomes more economical than long-term dialysis despite higher initial costs. — Source: Sage Journals, 2024
Kidney transplantation is often considered more cost-effective than long-term dialysis despite higher initial treatment costs.
What Are the Risks and Complications of Dialysis?
Dialysis complications include infections, low blood pressure, heart problems, and access-site complications.
First, repeated dialysis sessions can strain the cardiovascular system over time. For example, some patients experience chronic fatigue and blood pressure instability after treatment sessions.
Additionally, dialysis access points can develop infections or clotting complications.
Common Side Effects of Dialysis
- Muscle cramps
- Sleep problems
- Weakness
- Itching
- Anemia
- Depression
- Low blood pressure
According to kidney health research, cardiovascular complications remain a major concern among long-term dialysis patients. — Source: PMC Study, 2022
What Are the Risks of Kidney Transplant Surgery?
Kidney transplant surgery carries risks including organ rejection, infection, bleeding, and medication side effects.
First, transplant rejection can occur when the immune system attacks the donor kidney.
For example, acute rejection episodes may require hospitalization and medication adjustments.
Long-Term Transplant Risks
- Organ rejection
- Increased infection risk
- Diabetes from medications
- High blood pressure
- Certain cancers due to immunosuppression
At the same time, most transplant complications can be managed effectively with regular monitoring and medication adherence.
Can Patients Switch From Dialysis to Kidney Transplant Later?
Many kidney failure patients begin with dialysis and later transition to kidney transplantation.
First, dialysis often stabilizes patients while doctors evaluate transplant eligibility and search for donors.
For example, patients may spend months or years on transplant waiting lists before receiving suitable donor kidneys.
Additionally, living donor transplants can reduce waiting times significantly.
Dialysis and kidney transplant are not competing treatments in many cases because dialysis often serves as a bridge to transplantation.
What Foods and Lifestyle Changes Are Required After Dialysis or Transplant?
Kidney patients require diet and lifestyle changes to support treatment outcomes and reduce complications.
Diet Changes During Dialysis
Dialysis patients often need:
- Lower sodium intake
- Reduced potassium foods
- Controlled fluid intake
- Higher protein consumption
For example, bananas, potatoes, and processed foods may require limitation depending on lab results.
Lifestyle After Kidney Transplant
Transplant recipients usually gain more dietary flexibility but still require healthy eating habits.
Important lifestyle habits include:
- Taking medications on schedule
- Avoiding smoking
- Maintaining healthy weight
- Exercising regularly
- Monitoring blood pressure
What Tools and Support Systems Help Kidney Patients Manage Treatment?
Kidney patients benefit from medical tools, support groups, and digital health resources that simplify treatment management.
First, medication reminder apps help transplant recipients maintain strict medication schedules.
Additionally, dialysis tracking apps allow patients to monitor:
- Fluid intake
- Blood pressure
- Weight changes
- Dialysis schedules
Helpful resources include:
- National Kidney Foundation
- Hospital transplant coordinators
- Kidney patient support communities
- Government dialysis assistance programs
Free tools such as medication reminder apps can improve treatment adherence significantly.
What Should You Discuss With Your Nephrologist Before Deciding?
Patients should discuss survival expectations, eligibility, costs, risks, and lifestyle impact before choosing dialysis or transplant.
Important questions include:
- Am I eligible for transplant surgery?
- How long is the waiting list?
- What dialysis option fits my lifestyle?
- What are the expected long-term outcomes?
- How will treatment affect work and travel?
Actionable Next Steps for Patients and Families
Early planning improves treatment success and reduces emotional stress for kidney failure patients.
Next, consider these practical steps:
- Schedule nephrologist consultations early
- Learn about transplant waiting lists
- Explore financial assistance programs
- Build a long-term support system
- Follow recommended kidney-friendly diets
By preparing early, you can make treatment transitions smoother and safer.
Conclusion
Dialysis and kidney transplant are both life-saving treatments for kidney failure, but they offer different long-term experiences and outcomes.
First, dialysis provides immediate support and remains essential for many patients who are waiting for transplants or are not eligible for surgery. At the same time, kidney transplantation generally offers better long-term survival, improved quality of life, and greater independence for suitable candidates.
Ultimately, the best choice depends on your overall health, lifestyle, financial situation, and medical eligibility. By discussing options with a qualified nephrologist and understanding both treatments clearly, you can make a more confident decision about your future care.
Written by: Sunny Kushwaha — SEO Blog Writer with 2+ years of experience, specializing in AI-optimized content.
Reviewed by: Medical Content Review Team — Experts in nephrology and kidney health education.
Disclaimer: This article was initially drafted using AI assistance. However, the content has undergone thorough revisions, editing, and fact-checking by human editors and subject matter experts to ensure accuracy.
